The influence of two World Wars
The influence of two World Wars
Developments in anaesthesia during World Wars I and II
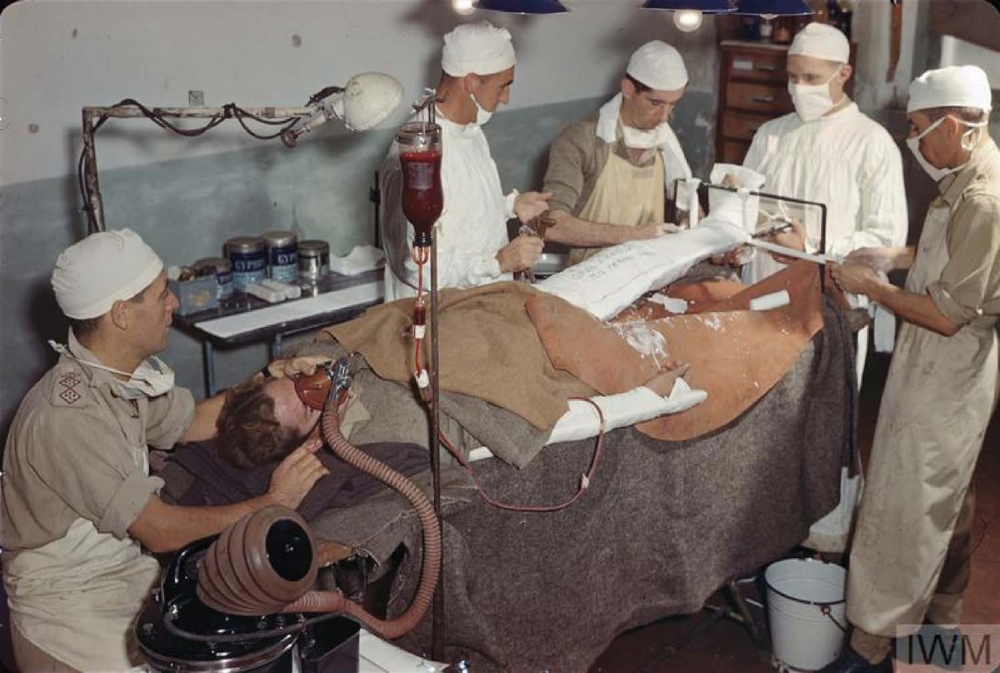
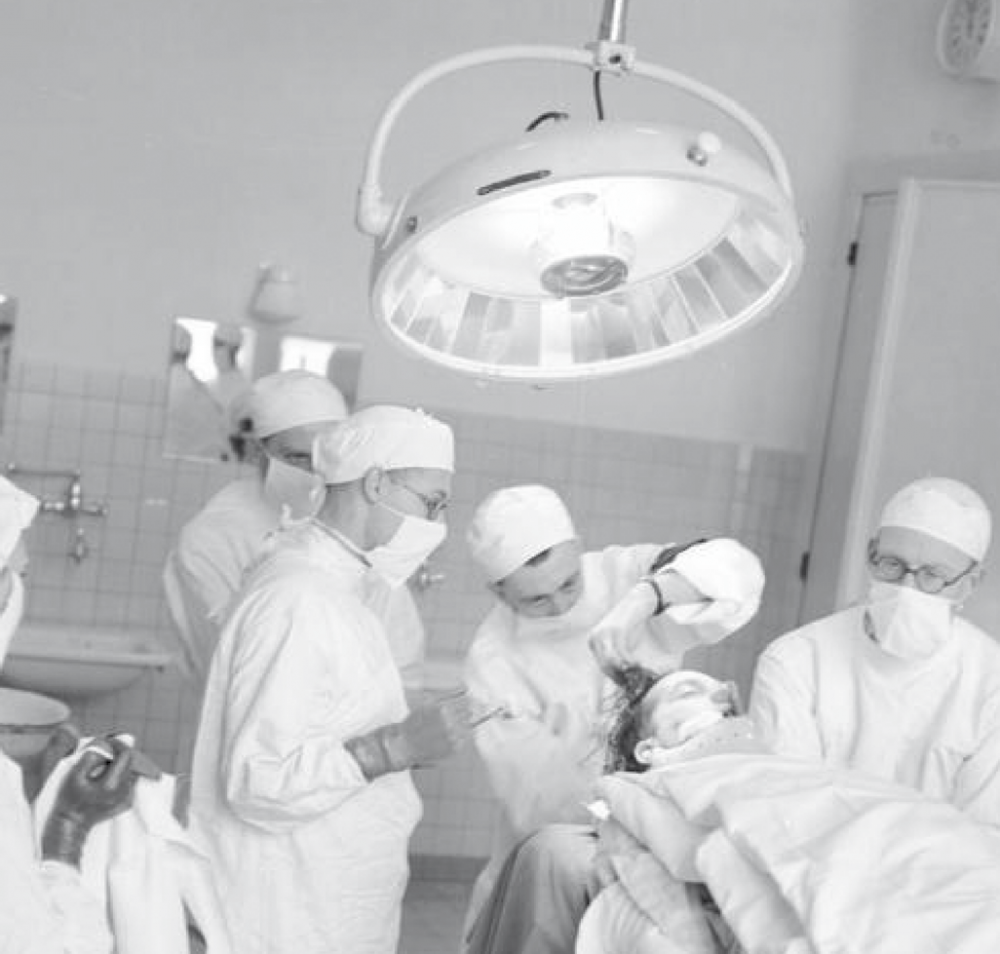
Surgeons, accompanied by a female nurse, in the operating theatre of a Casualty Clearing Station RAMC [© IWM (Q 26636)]
The lives of the Foundation Board’s members spanned the years 1888 to 2008, and inevitably they were touched by the events of the 20th Century’s two World Wars. These conflicts were perhaps the greatest man-made catastrophes of all time, but there is no doubt that ‘anaesthesia’ advanced as a specialty as a result of both. That advance is well illustrated by considering the specific involvements of the members of the first Board.
World War One
In 1914 the age of recruitment was 19, meaning that five of the Foundation Board’s members were eligible to serve at the start of the war, and another five became so before its end. Of these ten, five had medical roles, and five were combatants.
Ivan Magill was the only one who had qualified before the war (in 1913), and he joined the Royal Army Medical Corps (RAMC) on its outbreak, becoming Medical Officer to the Irish Guards. Archibald Marston qualified in 1915 and then joined the Royal Navy, serving as a Temporary Surgeon Lieutenant. Stanley Rowbotham joined an infantry regiment initially, but was advised to complete his training; he qualified in 1915 and was commissioned into the RAMC. Langton Hewer qualified in 1918 and served in the RAMC towards the end of the war. Reginald Pleasance did not qualify until 1919, but interrupted his studies to become a Surgeon Probationer in the Royal Navy, in which role he practised medicine, including the administration of anaesthetics.
Of the five combatants, four were medical students in 1914, but they interrupted their studies to serve. John Challis was already a lieutenant in the Territorial Army (Royal Field Artillery) so was called up at the outbreak of the war and served throughout. Alexander Low was a Gunnery Officer who received the Military Cross. Frankis Evans signed up to the Royal Naval Volunteer Reserve.
John Gillies was called up into the Highland Light Infantry, spent seven months as a prisoner of war and was another recipient of the Military Cross. Robert Macintosh, a New Zealander, was one of those many young men from Commonwealth countries who came to Britain to volunteer. Commissioned in the Royal Scots Fusiliers in 1915 he soon transferred to be a pilot in the Royal Flying Corps. Shot down over France and taken prisoner, he made three escape attempts, and was mentioned in dispatches in 1917.
The legacy of World War One
Before the Great War there were few specialist anaesthetists in either civilian or military practice, with most anaesthetics performed by 'generalists’ using very simple methods. General anaesthetic agents used were a mixture of ether, chloroform and ethylchloride administered via a Schimmelbusch mask and nitrous oxide. Spinal anaesthesia was another option using local anaesthetics such as stovaine, usually performed by the surgeon without the presence of an anaesthetist. One of the lasting legacies of the war was the recognition that the type of anaesthetic given should be tailored to the condition of the patient.
The Medical Research Committee Investigative Committee on Shock was beginning to uncover the difference between haemorrhagic shock, septic shock, primary and secondary shock and the role of acidosis, temperature and fluid replacement therapy. At the same time there were advances in the use of blood transfusions, with improved compatibility and the introduction of citrate stored blood. A physician and respiratory physiologist from Guys, called Geoffrey Marshall, developed the concept of anaesthetists as perioperative physicians. Using the understanding of the relevance of physiological observations, he developed recommendations for the choice of anaesthetic depending on the type of wound and the condition of the patient, for example patients with septic shock tolerated spinal anaesthesia because they were already vasodilated but those with haemorrhagic shock did not.
Before the war Gwathmey had developed a machine for administering nitrous oxide and oxygen, which included a device to measure the flow of gases. Marshall recognised that nitrous oxide was valuable as an anaesthetic agent in difficult cases and developed his own machine for administering the gas, adding bottles for the addition of ether and chloroform. Both of these machines were adapted post war by Captain Henry Boyle to create the Boyle’s machine that is so familiar to present day anaesthetists.
By the end of the war the concept of a surgical team and a resuscitation team was well established with an anaesthetists being an important integral part of the team. Although the anaesthetic agents did not change much over the course of the war the training of anaesthetists, the development of equipment and the perioperative care of the patient improved exponentially. These rapid developments directly affected
the career choices of two of our subjects with Hewer developing an interest in anaesthesia through working in the RAMC with Torrance Thomson of Edinburgh who had an original continuous gas flow ‘Gwathmey’ anaesthetic machine. Pleasance took the expertise he had gained as an anaesthetist back to Sheffield and was even paid for his services while still a medical student.
However, the influence of the war continued after 1918 and perhaps the greatest legacy arose after two RAMC Officers, Magill and Rowbotham, were posted to Queen’s Hospital for Facial & Jaw Injuries, Sidcup. Initially they did not have specific duties, but there was a need for anaesthetists to work with Major (later Sir) Harold Gillies to treat soldiers with complex maxillofacial injuries. They took up the almost contradictory challenges of allowing surgical access while maintaining and protecting the patient’s airway. Thus started a career-long collaboration in the development of airway devices, breathing circuits, connectors and inhalational delivery systems. This work was the very foundation of modern anaesthetic equipment as we know it still today, and it is impossible to overestimate its importance.
World War Two
After the first war the numbers of specialist anaesthetists in Britain started to grow slowly but surely as those doctors with the interest and expertise showed surgeons and patients the benefits that they could provide. The establishment of the Association of Anaesthetists in 1935 was both a marker of this growth and an indication of the determination of its existing practitioners to place the specialty on a proper footing. By 1939 all but two of the subsequent members of the first Board were fully established in anaesthetic practice, the exceptions being Ronald Woolmer, who was already a trainee, and Edgar Pask, who did not join the specialty until 1940. None served as combatants during this war, but all served in either civilian hospitals, under the banner of the Emergency Hospital Service (EHS), or in the medical branch of one of the three armed services.
Their numbers were divided equally between the two groups, with the younger ones under 40 predominating on active service, but with exceptions. As in all walks of life, health issues or the need to protect civilian services could prevent younger people joining up, and the need to provide specialist expertise would lead to recruitment from the older group. Marston, Magill, Langton Hewer, Low, Evans, Gillies, Katharine Lloyd-Williams, Bernard Murtagh, Alec Musgrove and Geoffrey Organe remained civilians throughout the war, usually leading the provision of anaesthetic services in their localities. In addition, Magill was appointed Anaesthetic Adviser to the EHS and Civilian Consultant to the Royal Navy, and Organe (exempt from war service because of recent surgery for colonic cancer) was an enthusiastic fire fighter, and served on major committees concerned with traumatic shock and with analgesia and anaesthesia in midwifery. Cecil Gray was accepted for military service in 1942 and posted to North Africa, but became critically ill with pneumonia and returned home to spend the rest of the war as a full-time anaesthetist in Liverpool.
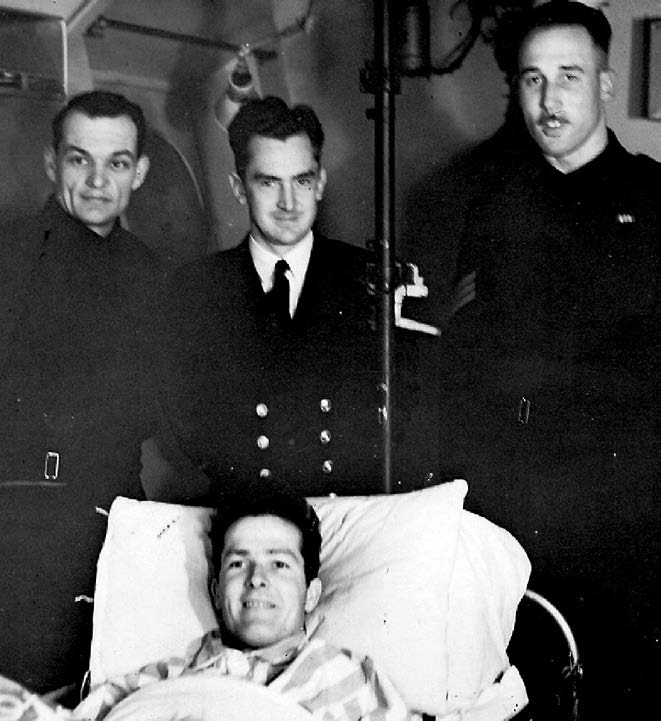
The others spent most of the war in uniform. Woolmer joined the Royal Naval Volunteer Reserve as early as 1939. He reached the rank of Surgeon Commander and was awarded the Volunteer Reserve Decoration. Most of the rest worked for a time in the EHS before (or after) serving in the RAMC, Vernon Hall being the senior example. First posted to Horton Hospital, he was recalled to King’s College Hospital at the start of the Blitz and then signed up for active service. Sent to the British Military Hospital in Colombo, Ceylon (now Sri Lanka) to establish a training programme for anaesthetists for the Indian and Burmese campaigns, he was, at one point, posted to a tented hospital in the jungle to train American soldiers for an invasion of Burma that did not take place! Appointed Adviser in Anaesthetics to the Eastern Command (Burma and South East Asia), he eventually rose to the rank of Brigadier in overall charge of anaesthesia in India and the Eastern Sector. At the end of the European war, his hospital, where his services were badly needed, successfully applied for his early release back to civilian duties.

Four achieved the rank of Lieutenant-Colonel: Pleasance was Adviser in Anaesthetics to the Southern India Command; George Edwards, having begun his war service with the EHS became Adviser in Anaesthetics to the British North African and Central Mediterranean forces, visiting anaesthetists throughout the zone; Henry Brennan became Adviser in Anaesthetics in the Middle East, based at the Scottish Hospital in Cairo; and Bernard Johnson served with distinction throughout the war, working in West Africa, the Middle East, Italy and Normandy, becoming Adviser in Anaesthetics to the Central Mediterranean Force, being mentioned in dispatches in 1944, and becoming civilian anaesthetist to the War Office after the war.
Surprisingly, given his seniority (in age, years of service and achievement) Rowbotham ended the war as a Major. Initially in charge of a surgical division, he was posted to the Cambridge Hospital, Aldershot where he led a School of Anaesthesia for Americans and received the US Bronze Star. After the Normandy landings he joined a maxillofacial unit in Belgium where his experience was invaluable, but his age led to immediate demobilisation with the end of the war in Europe. The most junior of the Board’s members in the RAMC was John Challis who, as a Captain, was posted to a mobile cerebral surgery unit in France at an early stage of the war. Within 15 days the unit was overrun by German forces and he spent three and a half years as a prisoner of war, giving many anaesthetics in primitive conditions.
The other two members of the first Board served with the RAF, Macintosh as an Air Commodore, becoming Director of Anaesthetics Services for both RAF and Royal Navy, but continuing to run the Nuffield Department in Oxford. War-time projects included training courses for service anaesthetists, and research into methods of artificial ventilation, the provision of respirable atmosphere in submarines, the design of life jackets to keep an unconscious pilot’s head above water, and the determination of the maximum altitude at which airmen could bail out without oxygen. Before the war he had spent time in Spain with plastic surgeons treating Civil War injuries and identified the need for a simple, portable vaporiser for use in conflict situations. This, with physicists Dr Kurt Mendelssohn and Dr Hans Georg Epstein, led to the development of the Oxford Vaporiser, produced at the Morris Motor works in Cowley, over 4,000 of which were delivered to military and civilian hospitals by the end of the war.
And finally there was Pask, who became a Junior Assistant in the Nuffield Department in 1940, and joined the RAF in 1941. Posted to the Physiological Laboratory (later the Institute of Aviation Medicine) at Farnborough he continued research he had started with Macintosh on life jacket design and hypoxia at altitude. Frequently he was the guinea pig for his own experiments, being anaesthetised and immersed in a swimming pool to test a design of life jacket or suffering acute hypoxia. He gained the reputation of the ‘bravest man in the RAF who never flew an aircraft’ and was awarded the OBE(Mil) in 1944 for his efforts. His one ‘failure’, probably fortuitous, was an attempt to develop an oxygen mask which would allow Sir Winston Churchill to smoke a cigar while being flown at altitude!
The Legacy of World War Two
At the end of the war specialists within each field of medicine and within each of the services were asked to reflect on the effect of the war on their specialty and provide a report, which was collated into a publication (see Note 2 below). Woolmer wrote the report on anaesthesia for the Royal Navy and Macintosh for the RAF. A common thread was that there had been a lack of commitment to anaesthesia between the wars and there were very few trained anaesthetists in post. Delegation of anaesthetic duties was the responsibility of the surgeons and even when doctors with anaesthetic experience were drafted in from the civilian population individual experience was often inadequate. Woolmer pointed out there was often only one medical officer on board ship, who would be a single handed operator and anaesthetist, relying on untrained assistants.
Consequently techniques used tended to be simple, with oxygen the only gas available and the use of regional techniques, especially spinal anaesthesia, varying considerably according to past experience. At the beginning of the war anaesthetists lacked the authority to order the equipment they needed and there was a tendency to send them obsolete, ‘old’ equipment such as a Clover’s Inhaler.
The appointment of Macintosh as an anaesthetic advisor to the war office in 1941 brought about changes including training courses, the appointment of anaesthetic advisors throughout the fields of war and recognition that anaesthetists are specialists and skilled. An anaesthetist was allocated to every unit with a surgeon and were assisted by well trained orderlies.
All three services reported advances in anaesthetic techniques with intravenous pentothal highlighted as of immeasurable value despite the experience at Pearl Harbour. Other advances mentioned were the use of endotracheal intubation, closed circuit anaesthesia, the Oxford Vaporiser, cyclopropane and the introduction of trilene.
Research throughout the war was driven by the need to improve the outcome for the patient. Further understanding of the causes and management of shock and development of the blood transfusion service led to all combatants having their blood group on their ID disc and the appointment of transfusion officers. Methods of estimating blood loss were developed based on the size of the injury and the appearance of blood on clothing and bandages, in addition to clinical observations. The value of administering oxygen in shock was recognised.
The Legacy for the Board of Faculty Members
Although all of the board members had survived the war sadly not all escaped the consequences. Pask died from a myocardial infarction in 1966 at the age of 54. His death was thought to be related to an injury sustained during his wartime experiments on hypoxia. Challis’ experience as a prisoner of war permanently undermined his health and he suffered increasing physical disability throughout his career, ultimately leading to his premature death from chronic lung disease in 1958.
The war had shown what academic anaesthesia could contribute in the way of teaching, training and research. Most of the future members of the board of the faculty remained or returned to pre-War appointments, albeit in senior positions. A number contributed to an expansion in academic departments. All of them were trained and experienced enough to be leaders of the new Faculty and take on more definitive roles within the new NHS. Together they had contributed much to the training of a large number of specialist anaesthetist for the Services who became available to fill consultant appointments in 1948.

Notes:
1 War Surgery 1914–1918, Chapter 3, Anaesthesia, Shock and Resuscitation, E Ann Robertson.
2 History of the Second World War: Surgery; Zachary Cope; Chapter 5 Anaesthesia
Further history articles are available here
